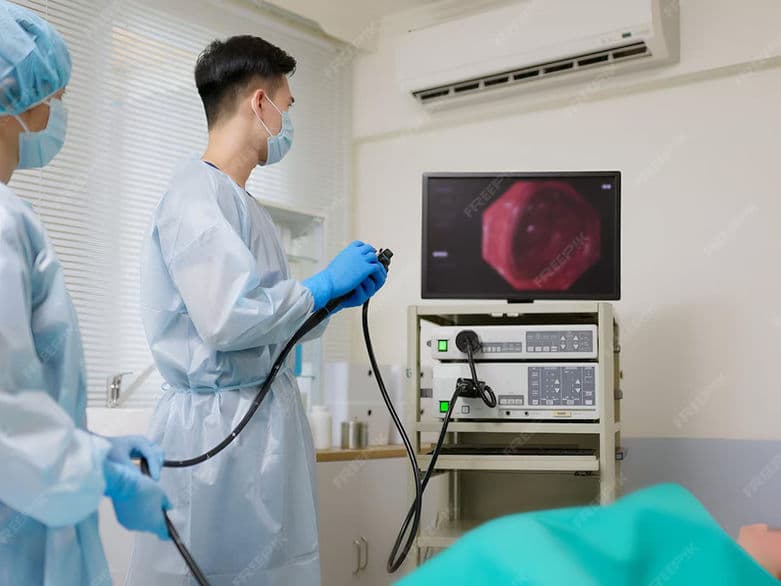
Colonoscopy
Colonoscopy
A colonoscopy is the definitive medical procedure used to examine the health of the large intestine (colon) and rectum. By using a colonoscope—a long, thin, flexible tube equipped with a high-definition camera and a light source—physicians can visualize the entire length of the colon in real-time. In 2026, this procedure is recognized globally as the "gold standard" for both the prevention of colorectal cancer through polyp removal and the diagnosis of complex inflammatory bowel conditions.
When It Is Recommended
Routine Cancer Screening: Medical guidelines now recommend that individuals at average risk begin regular screenings at age 45.
Rectal Bleeding: Investigating the source of bright red blood or dark, tarry stools.
Changes in Bowel Habits: Evaluating persistent diarrhea, chronic constipation, or a change in stool consistency that lasts more than a few weeks.
Unexplained Abdominal Pain: Searching for structural issues, inflammation, or growths that cause chronic discomfort.
Unexplained Weight Loss or Anemia: Identifying potential malabsorption issues or hidden internal blood loss.
High-Risk Surveillance: Frequent monitoring for those with a family history of colorectal cancer or genetic syndromes like Lynch Syndrome.
Conditions That Require Specialized Care
Inflammatory Bowel Disease (IBD): Patients with Ulcerative Colitis or Crohn’s disease who require "dye-spraying" (chromoendoscopy) to spot subtle tissue changes.
Large or Complex Polyps: Cases where polyps are located in difficult-to-reach folds, requiring advanced "Endoscopic Mucosal Resection" (EMR).
Previous Abdominal Surgery: Individuals with significant scar tissue (adhesions) that may require the use of a specialized "pediatric" or ultra-slim colonoscope.
Diverticulosis: Monitoring for complications in patients with multiple small pouches in the colon wall.
Chronic Anticoagulation: Patients on high-strength blood thinners who require a coordinated plan to manage bleeding risks during polyp removal.
[Image showing the path of the colonoscope through the entire length of the large intestine]
How a Colonoscopy Is Performed
The "Prep": To ensure total visibility, patients follow a clear liquid diet and consume a laxative solution the day before to completely empty the colon.
Sedation: Most procedures utilize "monitored anesthesia care," ensuring the patient is in a deep sleep and feels no discomfort throughout the exam.
Insertion and Inflation: The scope is gently inserted through the rectum. Small amounts of carbon dioxide or air are used to inflate the colon, smoothing out folds for a better view.
AI-Assisted Detection: Modern monitors utilize Artificial Intelligence (CADe) that acts as a "second set of eyes," highlighting potential polyps in real-time with high accuracy.
Polypectomy: If a precancerous growth (polyp) is found, the doctor passes a wire loop through the scope to "snare" and remove it instantly.
Biopsy: Small samples of tissue can be taken from inflamed areas to be analyzed for microscopic diseases.
Innovations in Colorectal Screening
AI-Powered Polyp CharacterizationBeyond just finding polyps, AI software now helps doctors determine in real-time if a polyp is likely to be precancerous, helping them decide the best removal technique.
Low-Volume "Palatable" PrepsThe development of concentrated, smaller-dose bowel preparations that are much easier to consume compared to the large-volume solutions of the past.
Water-Exchange ColonoscopyA technique that uses water instead of air to navigate the colon, which can reduce post-operative bloating and improve the success rate of the exam.
Self-Propelled Robotic ScopesExperimental "crawling" scopes that can navigate the colon with minimal pressure on the intestinal walls, potentially reducing the need for deep sedation.
High-Link 4K ImagingUltra-high-definition camera systems that allow doctors to see the microscopic "pit patterns" of the colon lining.
Green-Light FluorescenceUsing specialized light filters to make the blood vessels of a tumor stand out against healthy tissue, ensuring no suspicious areas are missed.
Pre-Procedure Preparation
Dietary Restriction: Switching to a low-fiber diet 3 days prior, followed by a 24-hour clear liquid diet (broth, plain gelatin, clear juices).
Hydration: Drinking plenty of clear fluids during the prep process to prevent dehydration and ensure the colon is thoroughly cleaned.
Medication Coordination: Discussing diabetes medications and blood thinners with the physician to safely manage dosages on the day of the procedure.
Transportation Arrangement: Because sedation is used, patients must have a designated driver to take them home after the procedure.
Prep Timing: Many clinics now recommend a "split-dose" prep (half the night before, half the morning of) for the cleanest possible results.
Diagnostic and Safety Monitoring
Adenoma Detection Rate (ADR): A quality metric tracked by physicians to ensure they are finding and removing polyps at or above national benchmarks.
Cecal Intubation Check: Confirmation that the doctor reached the very beginning of the colon (the cecum) to ensure a complete exam.
Withdrawal Time: Ensuring the doctor spends at least 6 to 10 minutes carefully inspecting the colon wall as the scope is removed.
Vital Sign Tracking: Constant monitoring of heart rate and oxygen levels by an anesthesiology professional throughout the procedure.
Why This Treatment Is Highly Effective
Prevents Cancer: Unlike other tests that only "find" cancer, a colonoscopy can actually prevent it by removing polyps before they turn into cancer.
Long-Term Protection: For average-risk patients with a "clean" exam, the protective benefits can last for up to 10 years.
Highest Accuracy: It is more sensitive and specific than stool-based tests or "virtual" CT colonographies for finding small or flat polyps.
Immediate Intervention: Diagnosis and treatment happen at the same time; if a problem is seen, it can often be fixed right then and there.
Direct Tissue Sampling: It provides the only way to get physical tissue samples for a definitive diagnosis of IBD or colitis.
Recovery and Aftercare
Immediate Post-Op: Patients rest in a recovery room for 30–60 minutes until the effects of the anesthesia have faded.
Managing Gas: It is normal to feel "gassy" or bloated for a few hours as the body naturally expels the air used during the procedure.
Return to Diet: Most patients can eat their regular meals immediately after the procedure, though starting with a light meal is often recommended.
Activity: No driving or operating machinery for 24 hours. Most people return to work and full activity the very next day.
Result Reporting: Visual findings are shared immediately, while results from biopsies or removed polyps usually take 5–7 business days.
Life After a Colonoscopy
The peace of mind that comes from a comprehensive, high-definition internal health check.
A significantly reduced risk of ever developing colorectal cancer thanks to the removal of precancerous growths.
A clear roadmap for future health, with a personalized schedule for when the next screening should occur.
For those with chronic bowel issues, the start of a targeted treatment plan based on the biopsy and visual data.
Empowerment to maintain digestive health through proactive, preventative medicine.