Esophagogastroduodenoscopy (EGD)
Esophagogastroduodenoscopy (EGD)
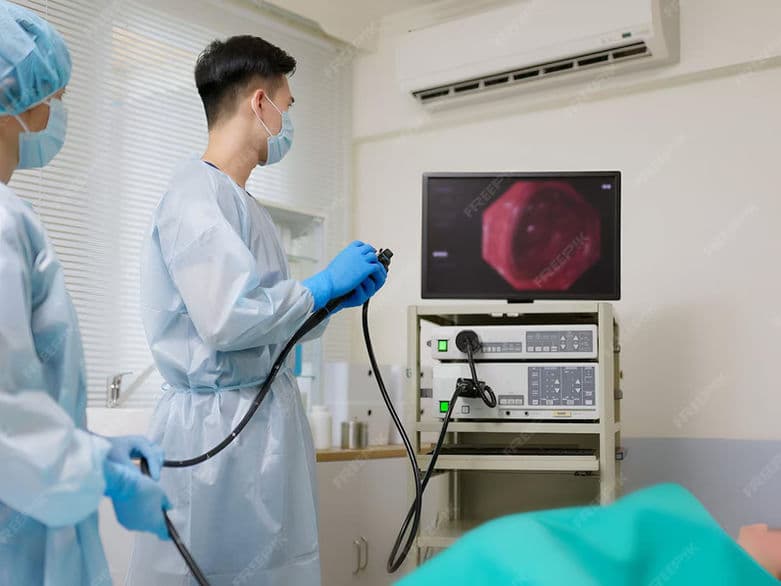
Esophagogastroduodenoscopy (EGD), commonly referred to as an Upper Endoscopy, is a minimally invasive procedure used to visualize the internal lining of the upper digestive tract. By using a thin, flexible tube equipped with a high-definition camera (endoscope), physicians can examine the esophagus, stomach, and duodenum (the first part of the small intestine) in real-time. In 2026, this procedure serves as the primary tool for both diagnosing digestive disorders and performing immediate therapeutic interventions without the need for traditional surgery.
Common Indications for EGD
Persistent Digestive Symptoms: Investigating chronic heartburn, acid reflux, or upper abdominal pain that does not respond to medication.
Difficulty Swallowing: Evaluating "dysphagia" or the sensation of food getting stuck in the chest.
Unexplained Weight Loss: Identifying underlying causes of malnutrition or malabsorption.
Anemia or Bleeding: Searching for the source of internal bleeding, often indicated by dark stools or low iron levels.
Nausea and Vomiting: Determining if structural blockages or ulcers are causing chronic gastric distress.
Celiac Disease Screening: Obtaining small tissue samples to confirm a diagnosis of gluten sensitivity.
Conditions That Require Specialized Care
Barrett’s Esophagus: Patients requiring regular surveillance to monitor for precancerous changes in the esophageal lining.
Portal Hypertension: Individuals with liver disease who need screening for "varices" (enlarged veins) that could lead to severe bleeding.
Esophageal Strictures: Narrowing of the esophagus from scar tissue that requires specialized dilation (widening) during the EGD.
Peptic Ulcer Disease: Monitoring the healing progress of deep sores in the stomach or duodenal lining.
Eosinophilic Esophagitis (EoE): A chronic allergic condition requiring multiple site-specific biopsies for accurate management.
[Image showing the path of the endoscope through the esophagus and into the stomach]
How an EGD Is Performed
Sedation: Most procedures utilize "conscious sedation" (monitored anesthesia care), allowing the patient to remain relaxed and comfortable throughout the process.
Throat Preparation: A local anesthetic spray is often applied to the back of the throat to suppress the gag reflex.
Insertion: The thin, flexible endoscope is gently guided through the mouth and into the esophagus. It does not interfere with breathing.
Insufflation: A small amount of air is pumped through the scope to inflate the stomach and duodenum, smoothing out the folds for a clearer view.
Biopsy and Intervention: If an abnormality is found, the doctor can pass tiny instruments through the scope to take tissue samples or remove polyps immediately.
Duration: The entire diagnostic portion of the procedure typically takes only 15 to 30 minutes.
Innovations in Upper Endoscopy
AI-Enhanced Lesion DetectionReal-time artificial intelligence software that highlights subtle changes in tissue color or texture, helping doctors spot early-stage cancers that might be invisible to the naked eye.
Disposable High-Definition EndoscopesThe transition toward single-use digital scopes in some facilities to eliminate the risk of cross-contamination and ensure the highest possible image resolution.
Magnification ChromoendoscopyUsing specialized light filters (like Narrow Band Imaging) to "stain" the tissue digitally, allowing for a microscopic view of the blood vessel patterns.
Hemostatic Powders and ClipsAdvanced "sprays" and mechanical clips that can stop an active stomach bleed instantly through the endoscope, avoiding emergency surgery.
Endoscopic Submucosal Dissection (ESD)A technique that allows surgeons to remove early-stage tumors from the stomach wall in one piece using the endoscope as a surgical platform.
Suturing DevicesTiny sewing machines attached to the end of the scope that allow doctors to close tears or perform "endoscopic sleeves" for weight loss.
Pre-Procedure Preparation
Fasting (NPO): Patients must have a completely empty stomach, usually requiring no food or drink for 6 to 12 hours prior to the exam.
Medication Management: Coordination regarding blood thinners, diabetes medications, or antacids that may need to be adjusted.
Transportation: Because of the sedation used, patients must arrange for a responsible adult to drive them home and stay with them for a few hours.
Informed Consent: Discussing the goals of the procedure and any specific symptoms the doctor will be targeting.
Dental Protection: A small plastic mouth guard is placed between the teeth to protect both the patient's dental work and the endoscope.
Diagnostic and Safety Monitoring
Oxygen Saturation: Constant monitoring of breathing and heart rate while the patient is under sedation.
Biopsy Analysis: Sending tissue samples to a pathologist to check for H. pylori bacteria, inflammation, or abnormal cells.
Post-Procedure Observation: A 30-to-60-minute recovery period where vitals are monitored as the sedative wears off.
Perforation Screening: A standardized safety check to ensure the integrity of the GI tract wall following any therapeutic interventions.
Why This Treatment Is Highly Effective
Direct Visualization: Unlike X-rays or CT scans, an EGD allows for a high-definition, true-color view of the tissue.
Two-in-One Capability: It functions as both a camera for diagnosis and a surgical tool for treatment in a single session.
Cancer Prevention: Identifying and removing precancerous polyps or treating Barrett’s esophagus can prevent cancer from ever developing.
Accurate Biopsies: Allows for targeted sampling of specific "hot spots," leading to much higher diagnostic accuracy than blind testing.
Immediate Results: In many cases, the doctor can share the visual findings with the patient immediately following the procedure.
Recovery and Aftercare
Sore Throat: A mild "scratchy" sensation in the throat is common for 24 hours; cool liquids and throat lozenges can help.
Gas and Bloating: Because air was used to inflate the stomach, patients may feel bloated until the air is naturally expelled.
Dietary Transition: Most patients can eat a light meal as soon as their gag reflex returns (usually within an hour).
Activity Limits: No driving, operating heavy machinery, or making major legal decisions for 24 hours due to the lingering effects of sedation.
Warning Signs: Patients are instructed to report any severe abdominal pain, fever, or difficulty breathing to their care team immediately.
Life After Upper Endoscopy
Clear answers regarding chronic pain or digestive distress, leading to a more effective treatment plan.
Peace of mind from ruled-out serious conditions, or the benefit of early detection for manageable issues.
Resolution of acute problems, such as stopped bleeding or cleared obstructions, during the procedure itself.
A simplified path to health with minimal "down time" compared to more invasive diagnostic surgeries.
Long-term health security through regular surveillance for high-risk conditions.